Changing practice: challenges & opportunities
The 2014 Care Act brought major changes in the requirements around care and support for adults, with the underlying duty for local authorities of ‘promoting wellbeing’ requiring a shift in approach. The Act also moved from specifying the provision of particular services, to requiring local authorities to ‘meet needs.’ Not only does this signal a move away from a limited menu of services to a more flexible and innovative approach to support, but it also established a focus on the particular needs and aspirations of people and the outcomes they want to achieve.
The language and concepts of personalisation, promoting independence, and prevention are by now well-established and familiar, but the experience of people receiving information, advice and assessment, and of care and support may still fall short in practice. This is relevant not just to what is offered to people, but how it is offered.
Why it is so difficult to get this change of approach right is worth exploring, particularly in the context of working with organisations trying to achieve practice improvement and better care and support outcomes. The constraints on achieving genuine change can be multiple, and inter-related, but are likely to include some or all of the following:
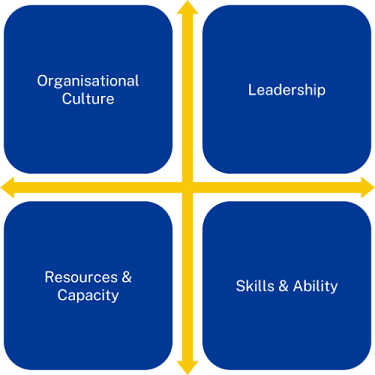
Organisational culture is a vague term, but it describes a range of beliefs, behaviours and shared values and principles which combine to set the framework for the overall style and character of local authorities and health partners. The culture can therefore be positive or negative; it can support innovation and encourage responsive and personalised support, or it can be reactionary and conservative. The culture will often be covert rather than explicitly stated, but it will be reflected by employees in the language and behaviours they demonstrate, and in the image of the organisation that they promote.
The resources available to public services will always be finite and usually under considerable pressure. This requires organisations to effectively ration services and support, but to do so on a fair, consistent and transparent basis. It is unacceptable – and illegal – to deny assessments of need to carers, or those they support, or to advise them that ‘there is no point’ to an assessment if they won’t get any support as a result of the process. Resources need to be seen more widely as those of the wider community, and of the social capital which exists within and between families and the community, in addition to the resources available through public services. The availability of ‘universal services’ which are open access and free or low cost for local citizens can significantly add to the resources available to help people manage their wellbeing.
The style of leadership is probably the most important influence on shaping overall organisational culture, and the features of the ‘brand’ of service that is on offer. Is it aspirational (wanting to do the best possible for citizens), or is it apparently more concerned with discouraging likely demands on resources? Are staff encouraged to act autonomously and flexibly, or are they required to adhere to rigid protocols and to have their decision making checked and their judgements queried?
The skills and abilities of staff will be directly and indirectly shaped by the organisational culture and messages from managers. For example, attempts to introduce better strengths-based assessments for carers, and to have an offer of support that is not just about eligibility, that can respond to carers’ needs other than by providing replacement care may be more likely to succeed under the following conditions:
- Decisions to offer flexible Direct Payments/Personal Budgets to carers to support personal outcomes can be made by social workers and approved by managers without needing higher approval by a Panel.
- Social workers have been trained to understand the carer offer, and are skilled in conversational assessment using open questions and active listening.
- The paperwork and recording requirements for the conversational assessment are fit for purpose and enable outcomes to be monitored over time.
- Social workers are well connected to community resources, or can work with community connectors to support people to use local resources and services to improve their health and wellbeing.
- Signposting to other support is explained and not just addressed by providing a leaflet or a list of web links or phone numbers.
- Social workers use reflective practice with colleagues to explore their response to carers’ needs and the outcomes achieved.
The importance of establishing a cultural shift and empowering staff to understand patients’ goals and priorities has also been a theme of the ‘What Matters to you?’ initiative in Scotland. This is intended to encourage more meaningful communication between people providing health and social care, and the people for whom they provide care and support. The focus on the importance of the relational aspects of care is consistent with the wider objectives of providing person-centred care. A multiple case study evaluation of approaches identified both barriers to implementation and enablers, and comments made by participants highlighted some of the experience. Undertaking a ‘What Matters’ conversation can be challenging, despite the professional experience of health and care staff, as this comment demonstrates:
“Asking ‘What matters to you?’ to patients means stepping out of your routine to do something odd and different. Not different in a huge way, but different enough to feel uncertain about it.” (P.19)
Feeling supported in using a ‘What matters’ approach was identified as a key enabler, as this comment also identifies:
“I have worked at other places so I’m very well aware of the strong teamwork ethics in this unit. I know that all of us are asking ‘what matters?’ every day, and that helps me feel more confident about doing it myself. You are just better on the floor when you feel supported.” (P.16)
Findings from the case studies overall identified positive outcomes, and in particular:
- People received care that was more relevant to their individual needs.
- Health and care services were delivered more efficiently.
- And staff members reported greater job satisfaction.
The biggest challenge identified was how to embed the approach into day-to-day practice. Or, how to move from a successful small-scale initiative, to achieving organisational cultural change.
IPC are currently working with a number of leadership teams supporting them to develop and embed their own bespoke principles for strengths-based working throughout their organisations. Part of our work includes a reminder of the DHSC guidance on strengths-based social work which set out a number of key characteristics of an organisation enabling a strengths-based approach:
- Strong leadership
- Shared commitment and accountability
- Promote working in a co-productive and collaborative way
- Trust in the workforce
- Support personalisation
- Ensure staff has the right information, tools, processes and systems
- Learning and development
- Focus on developing the strengths of the workforce
- Measure outcomes and quality
- Continuous improvement
This first bullet is the challenge that is key to leadership development work more broadly, and the necessity to ensure that the four components of culture, leadership, resources and skills are brought into alignment and form a mutually reinforcing virtuous circle.
If you would like to know more about our bespoke leadership development programmes and our work in this area, please contact Philip Provenzano, IPC Assistant Director.


